News
Take extra care to protect children from diarrhoea
Extremely hot weather can be intolerable, but it is young children who often bear the brunt of it. The very hot conditions experienced in many parts of the Western Cape has led to a noticeable increase in the number of children brought to Western Cape Health’s facilities with symptoms like diarrhoea, dehydration, and pneumonia.
Annually November to March marks a spike in children treated for diarrhoeal disease, and as we enter February (usually the hottest month), the Department is advising adults to be extra watchful over children. When your child has a runny tummy he/she may have diarrhoea.
Unclean hands can spread viruses that cause diarrhoea. During hot summer days, food can easily get spoilt. If eaten, this can also cause diarrhoea, which can cause to dehydration. As children can dehydrate very quickly, it can be life threatening.
Red Cross War Memorial Children’s Hospital’s Associate Professor Heloise Buys (Head of Clinical Unit Ambulatory & Emergency) says among the many reasons why diarrhoeal disease affects young children more seriously, is the fact that babies and young infants are completely dependent on their caregivers and mothers to feed them and to give them all the fluids they need. “They often can’t verbalise that they are thirsty. Also, because they are so much smaller than adults, losing a small amount of fluid in their watery stools is a big deal. They more easily become dehydrated or go into shock,” says Buys.
“Take the sign of the first loose stool seriously and immediately start with ‘replacement Oral Rehydration Solution’,” says Buys. You can make the solution at home: Boil a litre of water and let it cool down. Add to the water eight teaspoons of sugar and half a teaspoon of salt. Give the child small sips of the solution. Continue feeding the child. Give the child small, frequent snacks. Diarrhoea can last 48 to 72 hours. Care for your child at home rather than sending him to the crèche or school.
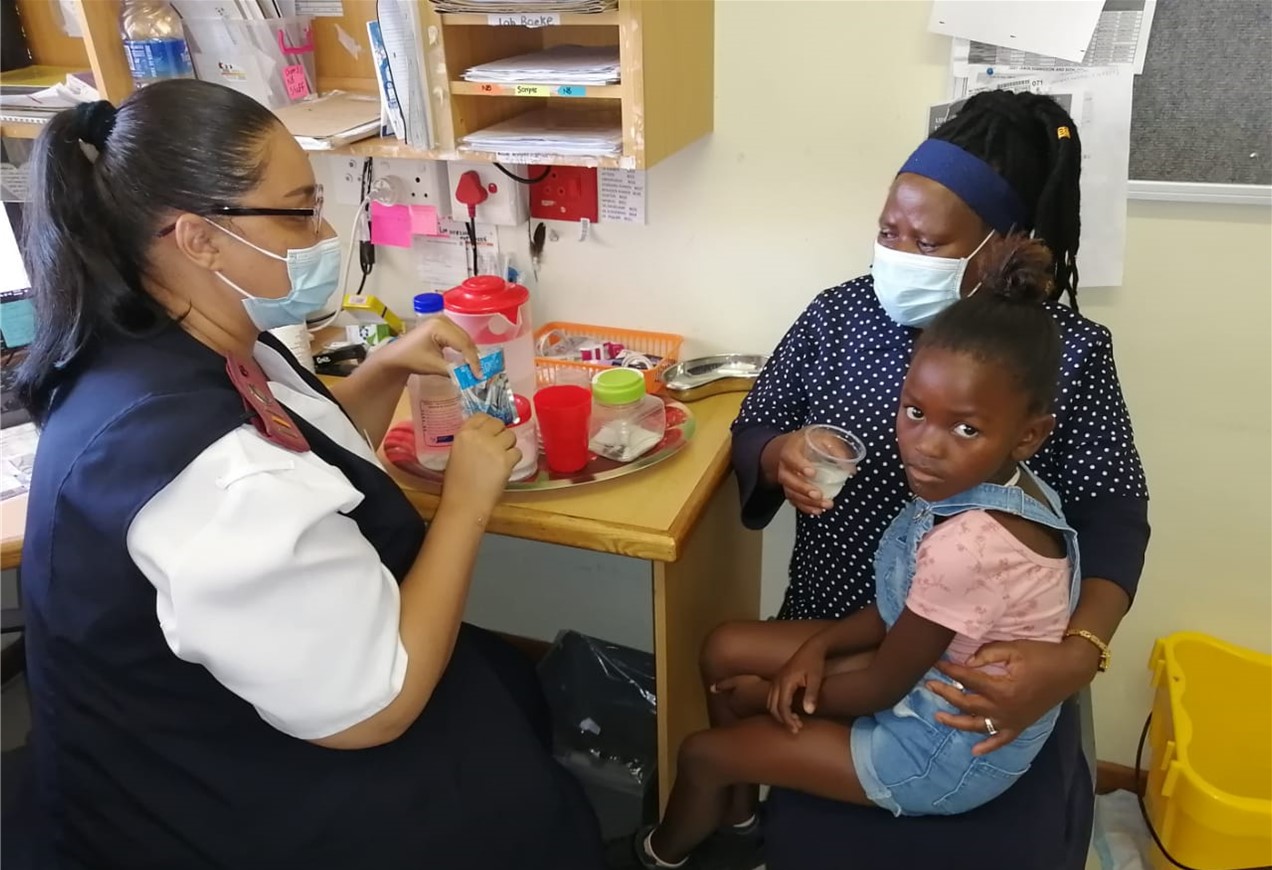 Sr Gale Goeieman of Tulbagh Clinic agrees on the importance of quickly acting to avoid dehydration. She has a couple of tips to encourage the child to drink the sugar-salt solution. “We advise mothers to preferably give it in a cup or feeding bottle – whichever works best. You can also mix a small amount of juice with the solution or add a small amount of the cool drink you usually make them, to the solution. If this does not work and the child is still not taking in fluids or vomiting all fluids they do drink, please come to clinic so that we can help to prevent severe dehydration,” says Goeieman.
Sr Gale Goeieman of Tulbagh Clinic agrees on the importance of quickly acting to avoid dehydration. She has a couple of tips to encourage the child to drink the sugar-salt solution. “We advise mothers to preferably give it in a cup or feeding bottle – whichever works best. You can also mix a small amount of juice with the solution or add a small amount of the cool drink you usually make them, to the solution. If this does not work and the child is still not taking in fluids or vomiting all fluids they do drink, please come to clinic so that we can help to prevent severe dehydration,” says Goeieman.
Danger signs that you should immediately get medical help, include:
- If there is blood in the child’s nappy or when they use the toilette,
- If the child vomits everything
- If the child is unable to drink or breastfeed
- If the child has tremors or shakes
- If the child is short of breath or has difficulty breathing
- If the child is not as alert as usual (the child is unusually quiet, not interested in their surroundings and not upright as usual)
Parents and caregivers can boost children’s health further by ensuring they receive their routine immunisations according to the Road to Health booklet, and that they are fed with breastmilk for as long as possible. Always keep your kitchen clean by using warm water and soap to wash surfaces, and teach children to wash their hands after using the toilet and before eating.
Sandra Maritz
Communications
Western Cape Government Health
Tel: 023 348 8100 or 071 589 1337
Email: Sandra.Maritz@westerncape.gov.za
Website: www.westerncape.gov.za


