News
Victoria Hospital celebrates discharge of longest ventilated Covid-19 patient
The story of Mr. Robson Shaby is one of hope and recovery in a time of overwhelming uncertainty. The 30-year-old Malawian gentleman overcame all odds to beat Covid-19 and became one of the first (and hopefully of many) critically ill recoveries in Victoria Hospital.
In mid-April Mr. Shaby was admitted to Victoria Hospital with severe Covid-19 pneumonia that resulted in him requiring increasing amounts of supplemental oxygen to help him combat the virus. He was admitted to the High Care Unit (HCU) at Victoria Hospital as the first Covid positive patient requiring long term critical care management. Due to the severity of the viral infection he ultimately required invasive mechanical ventilation and was ventilated for almost 4 weeks. Due to the hard work of the medical team, ICU nurses, anaesthetists, allied professionals and support staff, Mr.Shaby was eventually able to be weaned off ventilation after 3 weeks.
Dr Caryl Hollmann, Head of Department of Anaesthesia, shares that there were multiple eventful times during his stay in ICU, especially afterhours. “If it were not for the dedication of the on-call physician and ICU staff, a different outcome may have occurred. Though Mr. Shaby initially also required a feeding tube and a tracheostomy, the hard work of our physiotherapists and dieticians meant that he could eventually have both removed and start speaking and eating for the 1st time in 3 weeks.”
Mr. Shaby was discharged from High Care to a general ward on Monday 22 June where he continued his rehabilitation and then finally discharged home on 30 June 2020. To date Mr. Shaby has been the first Covid positive ventilated patient and the longest ventilated patient in Victoria’s HCU(typical length of stay would be less than 3-5 days). Knowing that the mortality rate of Covid pneumonia requiring ventilation is above 60%, his recovery is remarkable and deserves recognition.
“This case has highlighted the Spirit of Victoria” shares Mr Vaughan, CEO of Victoria Hospital “What I am hearing and experiencing, highlights the bond that exists between staff at Victoria. It was a huge collaborative effort among various staff members and we wish to highlight this and thank our staff for their investment”
Dr Graeme Hofmeyer, Family Medicine Registrar, shares the same sentiment: “I was amazed at how many people were looking after Robsyn Shaby. Everyone in the hospital knew who he was, and had some involvement in looking after him.”
Both Mr Shaby and his younger brother are extremely thankful to the staff at Victoria Hospital for their care and commitment. “Firstly, I thank God for what happened, and then I thank the team at Victoria Hospital. The doctors were amazing, they helped me a lot.” Mr Shaby reports that he is not sure how he contracted the virus. After going for a test, he spent a week at home in isolation, but when his symptoms worsened, he went to the nearest clinic for assistance as he was struggling to breathe. It was then that he was transferred to Victoria Hospital.
Dr. Priya Arnad, Medical Registrar who admitted Mr. Shabby upon arrival at Victoria shares, “He was incredibly young…we all wanted to do our best for him, and we wanted to ensure that he returned home as a contributing member of society. He had a big fighting spirit and that allowed the team to help him to come out of this.”
Dr. Clint Cupido, consultant in Medicine was astounded when considering the extent to which various health workers were involved. “To think that from the time he left his home, he would have encountered the ambulance crew involved, the staff in the emergency unit, the various shifts of nursing staff at the hospital, the daily cleaning staff... and many more. A case like Robson’s makes me realise how almost everyone in medicine and anaesthetics were involved at some point and the ability that we had to work closely with our colleagues in anaeasthesia. Ultimately these colleagues made a huge impression on his care. His positive outcome is a sign of how a hospital system actually works… our system DOES work. And we hoping to see more patients with this positive outcome.”
Dr Nasief van der Schyff, Head of Department of Medicine points out that the story of High Flow Nasal Oxygen therapy deserves some mention as this particular case predated the use of High Flow in the Southern Western Substructure. High Flow had been used historically at Victoria Hospital by the peadiatricians. The aneathetists and physicians had never used high flow prior to Covid. A machine was present in the paediatric ward. “We had a few informal discussions as part of the management team, but it had not been standard practice at the time.”
The day after Mr Shaby was admitted to hospital, a rep from the company that issued the machines gave some of the staff a demo. That same afternoon Dr. Cupido, informed the team that there was a 33-year old patient, profoundly hypoxic. “We knew that Tygerberg Hospital had been successfully using high flow oxygen on this kind of patient” said Dr van der Schyff. “We were a month into the pandemic and we had heard that the mortality from ventilation was poor. That’s when the decision was made to give it a try.” With the help of the rep donning PPE, and who also graciously donated the attachments needed to ensure that the machine could be used, the machine was set up in high care and a final tutorial was given.
Dr Van Der Schyff shares that It’s taken a pandemic to discover several firsts in the hospital. “Several firsts in terms of what we have done, how we have done things, how we have tried to be innovative, how the relationship between management and staff has been the best ever. Importantly the multi-disciplinary collaboration across the board. This is what the hospital has required, its required a whole hospital response. Mr. Shaby is one of example of what is possible from this hospital.”
Dr Caryl Hollmann, Head of Department of Anaesthesia explains that in the last ten years, the maximum period for intubation would be three to five days. This was the first intubation that was done for a patient that was going to stay for such a long period of time. “It was scary intubating someone my age. To put someone on a ventilator and consequently fear the unknown once he is on was not easy. There was limited data, we assumed the outcome will not be good and at times I would think that I may be the last person he would see.” When asked about what motivated the team while navigating unchartered waters, Dr. Hollmann shares she remembers thinking, “if we could just do it! If we could be that one unit in a small hospital that managed to intubate their first patient and get him through it. Our whole mindset was that it simply just HAD to happen!”
Dr Andy Heald, Medical Officer in Anaesthesia who was predominantly involved in Mr Shaby’s care during the day as part of the high care team, is also the first doctor to intubate a covid positive patient at Victoria hospital. He shares how collaborative the process was and yet unfamiliar at the same time. “There was so much we didn’t know. It was extremely rocky, we are used to seeing patients of his age group bouncing back quickly, but for him it was a slow process. It has taught me personally a lot about patience with this disease. It taught me how this is very much a disease of two steps forward, three steps back, and when it feels like you are losing the battle, something good happens and you have hope again. It was a test of our patience and resilience. What I have noticed with subsequent patients that we have got in the high care unit that require high flow oxygen or ventilation is that it is evident that we have learnt a lot from our time with Mr. Shaby. We certainly are a lot better and are well versed in dealing with patients of this nature.
It’s given us a lot of hope, that we can pull these patients through despite the odds being stacked against them.”
Sr. Wendy Bilby, Operational Manager for the nursing team in the High Care Unit expresses praise for the team of amazing people that she has worked with. “Everybody gave their all, we all got involved, it was very emotional, very intense and very rewarding, we learnt a lot. I am proud of all my colleagues.”
End -
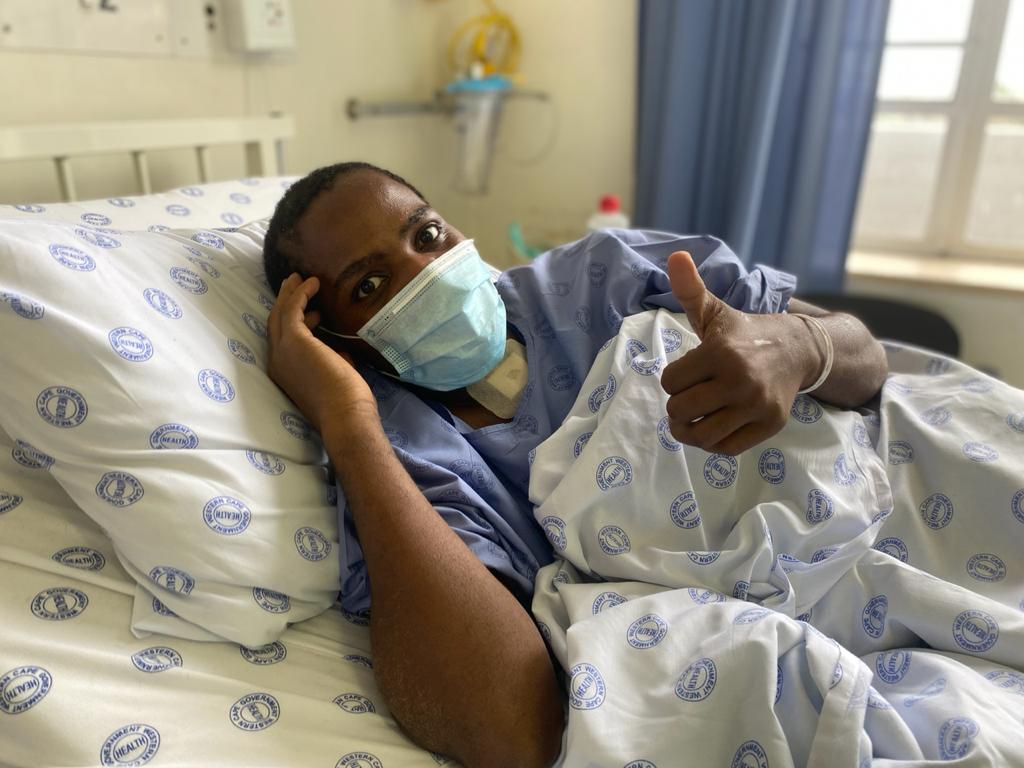
Image one: Mr Robsyn Shaby, the first Covid patient on ventilation at Victoria Hospital.
Image two: The core team involved in nursing Mr Robson Shaby back to health. Dr Graeme Hofmeyer, Sr. Wendy Bilby, Dr Andy Heald, Dr Caryl Hollmann, Dr Clint Cupido, Dr Graeme Dunbar, and Dr Nasief van der Schyff.
Natalie Watlington
Principal Communications Officer: Southern Western Sub-structures
Department of Health
Western Cape Government
Tel: 021 202 0947
Mobile: 081 277 0516