Osteoporosis
What is osteoporosis?
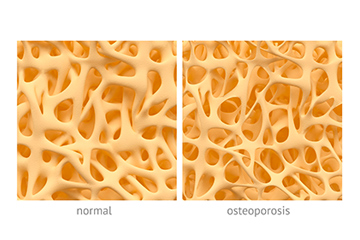 Osteoporosis is when your bone density and quality of bones deteriorate. This causes bones to become weak and fragile, which are prone to breaking easily, even as a result of a minor fall, a bump, a sneeze, or a sudden movement.
Osteoporosis is when your bone density and quality of bones deteriorate. This causes bones to become weak and fragile, which are prone to breaking easily, even as a result of a minor fall, a bump, a sneeze, or a sudden movement.
Fractures caused by osteoporosis can be life-threatening and a major cause of pain and long-term disability.
Strong bones, together with strong muscles, will help you enjoy an active, mobile and independent future. Your future quality of life can be determined by the state of your bone health.
It’s a fact that women over 45 years of age spent more days in hospital because of osteoporosis than many other diseases, including diabetes, heart attack and breast cancer.
Hip fracture facts
- Hip fractures are serious, and can be life-threatening.
- Hip fractures often result in the need for assisted care, and loss of physical independence.
- Fewer than half of those who survive a hip fracture regain their previous level of function. Approximately 20-25% of people who suffer a hip fracture die within a year.
Osteoporosis is a worldwide problem, and in many countries, up to 1 in every 3 women and 1 in 5 men aged 50 years or over will suffer an osteoporotic fracture.
What are the symptoms of osteoporosis?
Bone loss is gradual and without warning signs until the disease is advanced. A person usually doesn't know that they have it until it's too late. Unfortunately, in many cases, the first real "symptom" is a broken bone. Loss of height with gradual curvature of the back (caused by vertebral compression fractures) may be the only physical sign of osteoporosis.
Osteoporosis is called the ‘silent disease’ because there are no real symptoms before it is very advanced.
 Misconceptions
Misconceptions
A big misconception is that only older women suffer from osteoporosis. The fact is that bone loss in women can begin as early as the age of 25. New studies have shown the prevalence of osteoporosis in men is higher than previously thought, with approximately 1 in 5 men affected.
How can osteoporosis and fractures be prevented?
Although some conditions are out of your control (such as family history), other factors can cause bone loss to happen faster. There are certain steps that you can take to help prevent and fight this ‘silent’ disease.
The first step is to adopt a bone-healthy lifestyle no matter how old you are.
- Take regular weight-bearing and muscle strengthening exercise.
- Eat a nutritious diet rich in calcium, protein, vitamin D and other important nutrients.
- Avoid unhealthy habits such as smoking or drinking too much alcohol.
However for people at high risk of fracture it’s not enough to only have a bone-healthy lifestyle to prevent osteoporotic fractures. If you’re at high-risk you’re likely to need osteoporosis medication in order to protect you against future fractures.
Risk factors that you can change
Smoking - people who smoke, or have smoked in the past, are at increased risk of any fracture.
Drinking too much alcohol – if you drink more than 2 units of alcohol a day you have a 40% increased risk of sustaining any osteoporotic fracture, compared to people who drink less or no alcohol.
Low Body Mass Index (BMI) – a BMI below 19 is considered underweight and a risk factor for osteoporosis.
Poor nutrition - malnutrition in seniors is a special concern, particularly because they are more susceptible to osteoporosis, falls and fractures.
 Vitamin D deficiency - Vitamin D is essential for bone health in that it helps the body absorb calcium. Few foods contain vitamin D and sunlight is not always a reliable source of vitamin D. Vitamin D deficiency is common in the elderly or in people who don’t regularly go outdoors. If you’re at risk or older than 60 years it’s best to take a supplement to help protect you in the case of falls and possible fractures.
Vitamin D deficiency - Vitamin D is essential for bone health in that it helps the body absorb calcium. Few foods contain vitamin D and sunlight is not always a reliable source of vitamin D. Vitamin D deficiency is common in the elderly or in people who don’t regularly go outdoors. If you’re at risk or older than 60 years it’s best to take a supplement to help protect you in the case of falls and possible fractures.
Frequent falls – 90% of hip fractures occur as a result of a fall. If you’re prone to falls you should take action by fall-proofing your home and improving your muscle strength and balance through targeted exercises.
Insufficient exercise - inactivity results in increased bone loss. That’s why it’s important to get regular weight bearing and muscle-strengthening exercise. Studies have shown that older adults who get less exercise are more likely to have a hip fracture than those who are more active.
Eating disorders - anorexia and bulimia which can result in extreme weight loss are dangerous for bone health.
Risk factors that you can’t change
The risk of osteoporosis is influenced by age, gender and ethnicity. Generally, the older you get, the greater your risk of osteoporosis. Women are more susceptible to bone loss than men.
Although some risk factors can’t be changed you should be aware of which factors may affect you. The following risk factors should prompt you to seek a bone health assessment:
Family history - Genetics and shared lifestyle and dietary factors will contribute to your peak bone mass and the rate of bone loss at older age.
Previous fracture - People who have already sustained an osteoporotic fracture are almost twice as likely to have a second fracture compared to people who are fracture free.
Certain medications - Some medications may have side effects that directly weaken bone or increase the risk of fractures due to falls.
Primary/secondary hypogonadism in men with low testosterone levels have low bone density, which can be increased through testosterone replacement therapy.
Certain medical disorders – Some diseases, as well as the medications used to treat the disease, may weaken bone and increase the risk of fractures.
Menopause/hysterectomy - Rapid bone loss begins after menopause when the protective effect of estrogen is reduced.
Are you at risk?
If you’re over the age of 50 years and you’ve one or more risk factors, then you should discuss these with your doctor and ask for assessment.
The following Community Health Clinics will be able to assist you.
For handy fact sheets and infographics please visit World Osteoporisis Day 2016
Love your bones


